Blog
How Obstetric Simulation Scenarios Improve Maternal & Neonatal Outcomes

Obstetric simulation scenarios are structured training experiences used in healthcare education to recreate real-world labor and delivery situations through advanced simulation technology. These scenarios give learners the opportunity to practice recognizing complications, performing interventions, and coordinating care for both mother and baby within a safe, controlled environment.
As maternal care becomes more complex, simulation is widely used across nursing programs, hospitals, and clinical training environments. By allowing teams to rehearse both routine deliveries and high-risk emergencies, obstetric simulation helps improve readiness, clinical performance, and ultimately maternal and neonatal outcomes.
What Are Obstetric Simulation Scenarios?
Obstetric simulation scenarios are realistic training exercises designed to mimic clinical events during pregnancy, labor, delivery, and postpartum care.
In these scenarios, learners respond to simulated patients experiencing labor progression or obstetric complications. The environment is designed to reflect real delivery room workflows, allowing learners to practice clinical decision-making, communication, and emergency response in real time.
Modern obstetric simulation programs often include:
- High-fidelity maternal simulators
- Realistic labor and delivery scenarios
- Team-based training exercises
- Instructor-guided debriefing
- Evidence-based obstetric protocols
These experiences allow healthcare providers to build the skills necessary to manage both routine deliveries and life-threatening complications with confidence.
Why Obstetric Simulation Training Is Critical for Maternal & Neonatal Safety
Complications during childbirth can develop rapidly and require immediate, coordinated action. Learners must recognize warning signs early and intervene quickly to protect both mother and baby.
Simulation training improves maternal and neonatal safety by helping learners:
- Identify early signs of obstetric complications
- Practice rapid emergency interventions
- Improve communication within delivery teams
- Develop clinical confidence before treating patients
- Strengthen decision-making during high-stress situations
Research published in the National Library of Medicine shows that simulation-based training helps improve provider preparedness and clinical outcomes during maternal emergencies.
Types of Obstetric Simulation Scenarios Used in Training
Healthcare education programs use a wide variety of obstetric simulation scenarios to prepare learners for both common and high-risk childbirth events.
These scenarios expose learners to situations they may encounter during clinical practice.
Postpartum Hemorrhage Simulation
Postpartum hemorrhage is one of the leading causes of maternal morbidity worldwide.
In postpartum hemorrhage simulation scenarios, learners practice:
- Recognizing excessive bleeding
- Initiating emergency protocols
- Administering uterotonic medications
- Coordinating rapid response teams
Repeated practice helps learners react quickly and effectively when hemorrhage occurs in real clinical settings.
Shoulder Dystocia Simulation
Shoulder dystocia occurs when the baby’s shoulder becomes lodged behind the mother’s pelvic bone during delivery.
Simulation scenarios allow learners to practice critical maneuvers such as:
- McRoberts maneuver
- Suprapubic pressure
- Rotational delivery techniques
These high-stress events are rare but require immediate intervention, making simulation an ideal training tool.
Neonatal Resuscitation Scenarios
Newborns may require immediate support after birth if they experience breathing or cardiac complications.
Neonatal resuscitation simulation scenarios train learners to:
- Assess newborn vital signs
- Initiate resuscitation protocols
- Perform airway management
- Coordinate care with neonatal teams
These scenarios help improve response times and confidence when caring for vulnerable newborns.
Preeclampsia and Eclampsia Simulation
Hypertensive disorders during pregnancy can escalate quickly and pose serious threats to both mother and baby.
Simulation training prepares learners to:
- Recognize signs of severe preeclampsia
- Administer magnesium sulfate
- Manage seizures during eclampsia
- Stabilize maternal vital signs during emergencies
How Maternity Simulation Scenarios Improve Clinical Training
Maternity simulation scenarios provide advantages that go beyond traditional classroom learning or clinical observation.
Safe Learning Environment
Simulation allows learners to practice procedures and make decisions without risking patient safety.
Exposure to Rare Emergencies
Some obstetric emergencies occur infrequently in clinical settings. Simulation ensures learners gain experience managing these high-risk situations.
Improved Team Communication
Labor and delivery require coordinated teamwork between nurses, physicians, midwives, and neonatal specialists. Simulation strengthens communication skills in high-pressure environments.
Consistent Training Experiences
Every learner can experience the same scenario, allowing educators to standardize training and ensure consistent outcomes.
Who Uses Obstetric Simulation Training?
Obstetric simulation scenarios are widely used across healthcare education and clinical environments, including:
- Nursing schools
- Midwifery training programs
- Doula certification programs
- OB/GYN residency programs
- Hospital labor and delivery teams
- Continuing education programs for maternal health professionals
For nursing students and early-career clinicians, simulation bridges the gap between classroom education and real-world clinical experience.
Technology Behind Modern OB Simulation
Advances in simulation technology have transformed how maternal healthcare training is delivered.
Today’s high-fidelity maternal simulators can replicate:
- Labor progression and cervical dilation
- Fetal descent and delivery mechanics
- Maternal vital sign changes
- Fetal heart rate monitoring
- Obstetric emergencies such as hemorrhage or dystocia
These immersive training environments allow learners to experience realistic childbirth scenarios while instructors monitor performance and provide feedback.
Elevate Healthcare OB Simulation Solutions
Healthcare institutions looking to strengthen maternal training programs often rely on advanced simulation technology to recreate realistic labor and delivery scenarios.
Elevate Healthcare offers advanced obstetric simulation solutions for healthcare education and hospital training environments.
Lucina – Advanced Maternal Birth Simulator
Lucina is a high-fidelity maternal simulator designed specifically for labor and delivery training.
Educators can use Lucina to recreate a wide range of obstetric simulation scenarios, including:
- Normal vaginal birth
- Postpartum hemorrhage
- Shoulder dystocia
- Breech delivery
- Maternal complications
- Neonatal resuscitation scenarios
Lucina provides realistic anatomy, responsive physiology, and immersive delivery mechanics that allow learners to experience childbirth scenarios that closely mirror real clinical environments.
Building a Complete Maternal Simulation Training Program
Many healthcare programs combine multiple simulation tools to create a comprehensive maternal and neonatal training environment.
Complementary simulation solutions include:
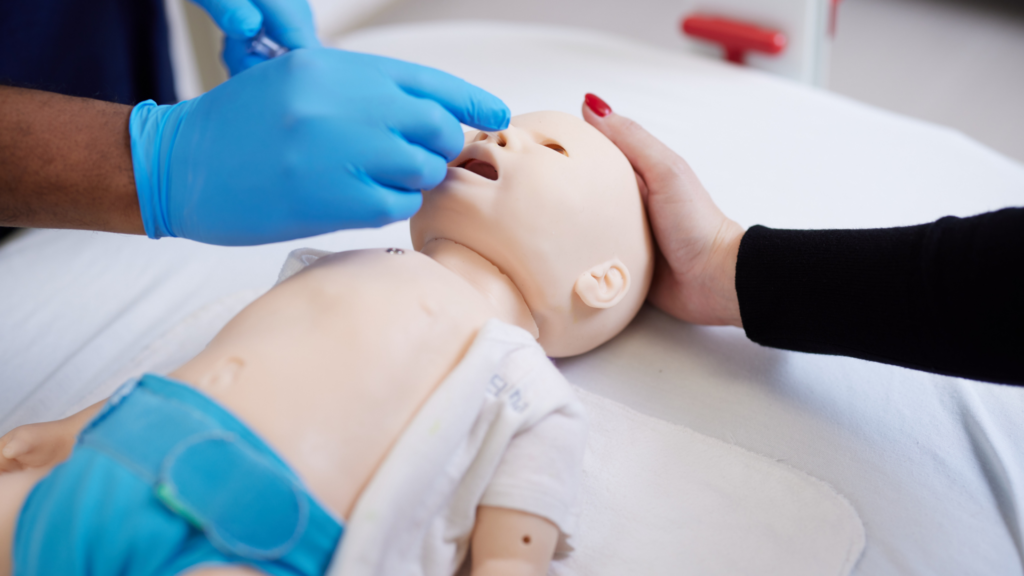
Luna – Newborn Care Simulator
Luna allows learners to practice newborn assessment and post-delivery care, supporting neonatal training following labor and delivery simulations.
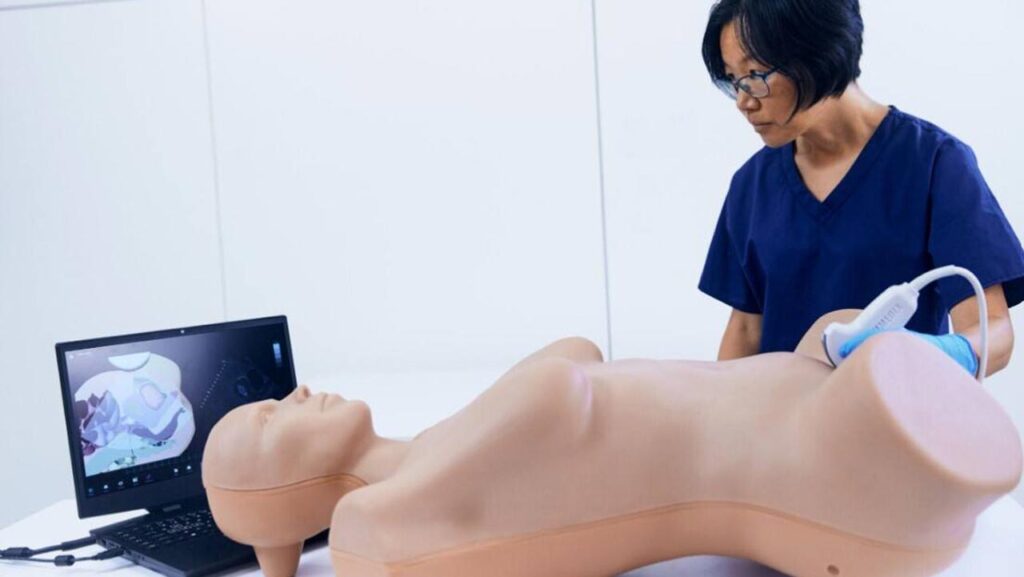
Vimedix – Ultrasound Simulator
Ultrasound is critical for prenatal assessment and fetal monitoring. Vimedix allows learners to practice ultrasound scanning and interpretation in a simulation environment.
Preparing Healthcare Teams for Safer Birth Outcomes
Improving maternal and neonatal outcomes requires healthcare providers who are confident, prepared, and able to respond quickly during childbirth complications.
Obstetric simulation scenarios give learners and clinical teams the opportunity to build these skills before encountering real emergencies. By practicing complex maternity scenarios in realistic environments, they develop clinical judgment, communication, and teamwork skills needed to deliver safe, effective care.
When implemented thoughtfully, simulation-based training supports measurable improvements across the continuum of maternal and neonatal care.